Tuberculosis was previously the primary cause of infectious spondylitis. Before the advent of effective chemotherapy, time and surgery for paralysis were the only treatment options. Tubercular bone and joint infections currently account for 2% to 3% of all reported cases of M. tuberculosis. Spinal tubercular infections account for one third to one half of the bone and joint infections. The thoracolumbar spine is the most commonly infected area. The incidence of infection seems to increase with age, but males and females are almost equally infected.
Pathologically, the infection is characterized by acid-fast–positive, caseating granulomas with or without pus. Tubercles composed of monocytes and epithelioid cells, forming minute masses with central caseation in the presence of Langerhans-type giant cells, are typical on microscopic examination. Abscesses expand, following the path of least resistance, and contain necrotic debris. Skin sinuses form, drain, and heal spontaneously.
Bone reaction to the infection varies from intense reaction to no reaction. In the spine, the infection spares the intervertebral discs and spreads beneath the anterior and posterior longitudinal ligaments. Epidural infection is more likely to result in permanent neurological damage.
Slowly progressive constitutional symptoms are predominant in the early stages of the disease, including weakness, malaise, night sweats, fever, and weight loss. Pain is a late symptom associated with bone collapse and paralysis. Cervical involvement can cause hoarseness because of recurrent laryngeal nerve paralysis, dysphagia, and respiratory stridor (known as Millar asthma). These symptoms may result from anterior abscess formation in the neck. Sudden death has been reported with cervical disease after erosion into the great vessels.

Neurological signs usually occur late and may wax and wane. Motor function and rectal tone are good prognostic predictors. Jain et al. calculated that the spinal canal can accommodate 76% encroachment on CT scan without neurological abnormality. investigators reported that 60% to 90% of patients with Pott paraplegia recovered with prolonged bed rest in an open-air hospital.
Laboratory studies suggest chronic disease. Findings include anemia, hypoproteinemia, and mild ESR elevation. Skin testing may be helpful, but is not diagnostic. The test is contraindicated in patients with prior tuberculous infection because of the risk of skin slough from an intense reaction and is not useful in patients with suspected reactivation of the disease.
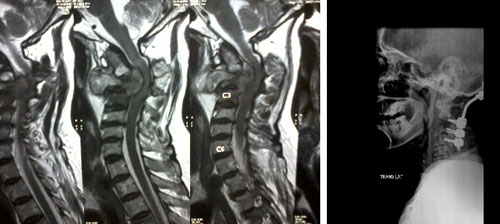
Early radiographic findings include a subtle decrease in one or more disc spaces and localized osteopenia. Later findings include vertebral collapse, called “concertina collapse” by Seddon because of its resemblance to an accordion. Soft-tissue swelling and its late calcification are highly predictable radiographic findings. CT scanning, with or without contrast, allows better evaluation of the pathological process and the degree of neural compromise. MRI permits further delineation of the pathological process. Abscess formation and the presence of bone fragments were the only MRI findings that helped distinguish spinal tuberculosis from neoplasia. None of these tests is confirmatory for tuberculosis, however. Scientist noted that 67 Ga scanning was most useful in patients with disseminated tuberculosis.
Definitive diagnosis depends on culture of the organism and requires biopsy of the lesion. Percutaneous techniques with radiographic or CT control usually are adequate. Epithelioid granulomas were seen in 89%, positive acid-fast bacilli cultures in 83%, and positive acid- fast bacilli smears in 52%. Open biopsy may be required if needle biopsy is dangerous or nonproductive or if other open procedures are required.
Delayed diagnosis and missed diagnosis are common. Differential diagnoses include pyogenic and fungal infections, secondary metastatic disease, primary tumors of bone (e.g., osteosarcoma, chondrosarcoma, myeloma, eosinophilic granuloma, and aneurysmal bone cyst), sarcoidosis, giant cell tumors of bone, and bone deformities such as Scheuermann disease.
Definitive diagnosis by culture of a biopsy specimen is important because of the toxicity of the chemotherapeutic agents and the length of treatment required. No patient developed paraplegia after surgery.
Better results with regard to deformity, recurrence, development of paralysis, and resolution when radical surgery is performed with chemotherapeutic coverage. The resolution of paraplegia did not depend on surgical intervention. Long-term bed rest, with or without cast immobilization, was ineffective. If the facilities for radical surgery are unavailable, ambulatory chemotherapy is the treatment of choice.
The indications for surgery in the absence of neurological symptoms vary widely. Involvement of more than one vertebra significantly increases the risk of kyphosis and collapse. Open biopsy for diagnosis, débridement, and grafting with or without anterior instrumentation may offer the most direct approach in these patients. Resistance to chemotherapy and recurrence of the disease are other indications for radical surgical treatment.
The indications for surgery in early or late disease as severe kyphosis with active disease, signs and symptoms of cord compression, progressive impairment of pulmonary function, and progression of the kyphotic deformity. Primary contraindications to surgery are cardiac and respiratory failure.
Posterior fusion, with or without spinal instrumentation, is indicated after anterior decompression and grafting to prevent late collapse and stress fracture of the graft if more than two vertebrae are involved and if anterior instrumentation is not used. Posterior fusion alone rarely is indicated at this time.
High incidences of failure and late progression of kyphotic deformity, with or without fatigue fracture of the fusion, have followed posterior fusion alone. Tricortical iliac crest is the preferred bone graft material for all levels, provided that it is long enough. External immobilization is mandatory whenever débridement and grafting are performed.
Halo (vest, cast, or pelvic) immobilization for 3 months is used after cervical and cervicothoracic procedures. Removable or nonremovable thoracolumbar immobilization is used after thoracic and thoracolumbar procedures until the grafts have completely healed (9 to ≥12 months). Lumbosacropelvic immobilization is used after low lumbar procedures and should be from the hip to the knee of at least one leg for 6 to 8 weeks, followed by thoracolumbosacral immobilization until the graft has healed, and the infection has resolved.
feel free to contact us!