Minimally Invasive Spine Surgery
Spine surgery is traditionally done as "open surgery." This means that the area being operated on is opened with a long incision to allow the surgeon to view and access the anatomy. In recent years, however, technological advances have allowed more back and neck conditions to be treated with a minimally invasive surgical technique.
Because minimally invasive spine surgery (MISS), does not involve a long incision, it avoids significant damage to the muscles surrounding the spine. Typically, this results in less pain after surgery and a faster recovery.
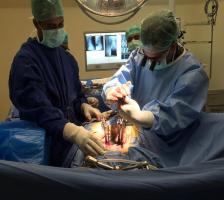
The indications for minimally invasive spine surgery are the same as those for traditional open surgery. Spine surgery is usually recommended only when a period of nonsurgical treatment — such as medications and physical therapy — has not relieved the painful symptoms caused by your back problem. In addition, surgery is only considered if your doctor can pinpoint the exact source of your pain, such as a herniated disk or spinal stenosis..
Minimally Invasive techniques
There are numerous minimally invasive techniques. The common thread between all of them is that they use smaller incisions and cause less muscle damage. Minimally invasive techniques can be used for common procedures like lumbar decompression and spinal fusion.
Decompression relieves pressure on spinal nerves by removing portions of bone or a herniated disk. Spinal fusion corrects problems with the small bones of the spine (vertebrae). The basic idea is to fuse together the painful vertebrae so that they heal into a single solid bone.
Open Surgery vs Minimal Invasive Surgery
One of the major drawbacks of open surgery is that the pulling or "retraction" of the muscle can damage both the muscle and the surrounding soft tissue. Although the goal of muscle retraction is to help the surgeon see the problem area, it typically affects more anatomy than the surgeon requires. As a result, there is greater potential for muscle injury, and patients may have pain after surgery that is different from the back pain felt before surgery. This can lead to a lengthier recovery period. The larger incision and damage to soft tissues may also increase both blood loss and the risk for infection.
Minimally invasive spine surgery was developed to treat spine problems with less injury to the muscles and other normal structures in the spine. It also helps the surgeon to see only the location where the problem exists in the spine. Other advantages of MISS include smaller incisions, less bleeding, and shorter stays in the hospital.
As opposed to open spine surgery, minimally invasive surgical approaches can be faster, safer and require less recovery time. Because of the reduced trauma to the muscles and soft tissues (compared to open procedures), the potential benefits are:
Benefit of Minimally Invasive Surgery over Open Surgery
- Better cosmetic results from smaller skin incisions (sometimes as small as several millimeters)
- Less blood loss from surgery
- Reduced risk of muscle damage, since less or no cutting of the muscle is required
- Reduced risk of infection and postoperative pain
- Faster recovery from surgery and less rehabilitation required
- Diminished reliance on pain medications after surgery
Risk Factors
In addition, some MIS surgeries are performed as outpatient procedures and utilize only local anesthesia — so there is less risk for an adverse reaction to general anesthesia.
As with any surgical procedure, no matter how minimal, there are certain risks associated that include, but are not limited to:
- Possible adverse reaction to the anesthetic
- Unexpected blood loss during the procedure
- Localized infections, no matter how small the incision area
And, though uncommon, there is always a small chance that the initial MIS surgery cannot be completed, requiring either a second procedure or full open surgery.
Conditions Treated Using MIS Procedures
- Degenerative disc disease
- Herniated disc
- Lumbar spinal stenosis
- Spinal deformities such as scoliosis
- Spinal infections
- Spinal instability including spondylolisthesis
- Vertebral compression fractures
- Spinal tumors
Candidates for MIS Surgery
A doctor will be able to tell which MIS surgeries, if any, might be an option for treating a spinal condition. In some situations, MIS surgery may not be as safe or effective as traditional open surgery. If so, the doctor will be able to inform you about the relative risks and benefits. In addition, there are some conditions that are not truly treatable with MIS surgery.
Success rate
Comparing minimally invasive spine surgery success rates with that of traditional surgery, research shows that minimally invasive spine surgery “MIS” has over 90% of success rate. You will be surprised to know that the success rate of traditional or open surgery is over 95%.
How long does it take to recover from minimally invasive back surgery?
Patients who undergo minimally invasive spine surgery (also sometimes referred to as less invasive spine surgery) tend to recover much faster than those who have an open spine surgery. Many people who have undergone minimally invasive spine surgery will be able to return to normal activities in approximately six weeks.